The CARD™ System: A patient-centred care tool to ease pain and fear during school vaccinations
Anna Taddio, Lucie M. Bucci, Charlotte Logeman, Victoria Gudzak
Anna Taddio PhD (1,2), Lucie M. Bucci MA (3), Charlotte Logeman MPH (1,2), Victoria Gudzak BSc, MSc(cand) (1,2)
1) Leslie Dan Faculty of Pharmacy, University of Toronto
2) The Hospital for Sick Children, Toronto
3) Immunize Canada
Corresponding author: Anna Taddio PhD
School-based (mass) vaccination programs are an effective way to reach a large number of youths to deliver recommended vaccines. However, the usual processes used to plan and deliver vaccinations at school are complex and do not systematically prioritize and address student needs and preferences (1). Failure to include students – the primary clients of school vaccinations – in the planning and delivery of vaccinations can have the unintended effect of undermining vaccination. This article reviews some of the ways current approaches to school vaccinations can cause harm and offers an evidence-based framework for planning and delivering vaccinations in school programs that addresses students’ needs and preferences.
Approximately two-thirds of students are afraid of needles and cite pain and associated fear as the worst part of school vaccinations (2). Fear is associated with a higher risk of fainting, which may cause serious injuries due to falling (3). These negative experiences with vaccination can interfere with the completion of the vaccination series and future vaccination in an attempt to avoid the needle. Evidence-based interventions currently exist to mitigate pain and fear (4); however, students are not benefiting from them because they are not systematically integrated into vaccination planning and delivery activities. For instance, vaccinations typically take place in large spaces such as the school gymnasium, where students are present in large numbers and are watching each other being vaccinated. Such settings and processes promote fear and fear contagion (spreading fear to others) and do not respect an individual child’s preference to be vaccinated in a private space, an option that is available in other vaccination settings. In addition, students are not formally educated ahead of time about how to cope with needle pain and fear and are often not permitted to bring coping strategies such as electronic devices, despite strong scientific evidence demonstrating that preparation ahead of time and use of coping strategies results in less pain and fear.
Beyond the vaccination procedure, teaching students coping skills has lifelong benefits, as they will undoubtedly encounter numerous other stressful situations in the future and can use these skills to cope with them. Action needs to be taken to systematically incorporate and prioritize evidence-based interventions into school vaccination programs. In the short term, these interventions have the potential to result in more positive experiences with vaccination because students will experience less fear, pain and fainting. In the long term, students may benefit from having more trusting relationships with health care providers, more positive attitudes towards vaccination, and a higher acceptance of vaccination.
In 2015, an evidence-based clinical practice guideline (CPG) for mitigating vaccine injection pain, fear and fainting was published (4). The CPG recommendations were incorporated into the Canadian Immunization Guide and formed the basis for the World Health Organization’s (WHO) first policy statement on this topic (5). In 2019, authors of the CPG developed a vaccination delivery framework called the CARD™ System that operationalizes the CPG’s recommendations for the school vaccination setting (6). Each letter of the word ‘card’ encompasses a category of evidence-based interventions (C-Comfort, A-Ask, R-Relax, D-Distract) to reduce pain, fear and fainting. Activities related to both the planning and delivery of school-based vaccinations are reviewed and altered to align with the principles of CARD™. There is a commensurate requirement for all individuals involved in the school vaccination program to be trained and versed in the framework.
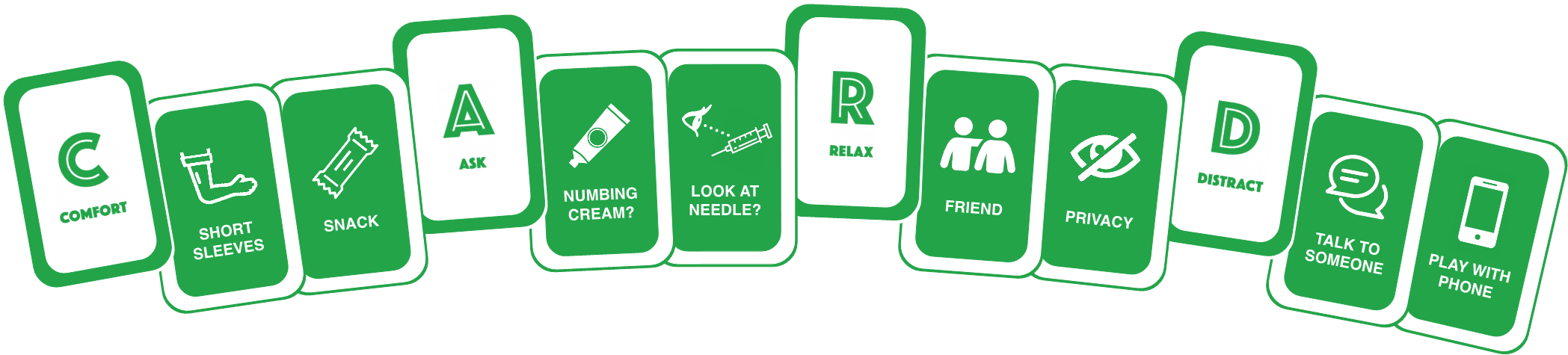
The key activities included in CARD™ are summarized in Table 1. Briefly, specific planning activities include, but are not limited to, meeting with school principals to secure optimal spaces for administering vaccinations and educating students in their classrooms ahead of time about CARD™ and the specific coping strategies they can use. On the day of vaccination, the clinic is set up to minimize cues that elicit fear (e.g., separate waiting area for students outside of the vaccination clinic, hiding of needles) and students are supported in using their preferred coping strategies during vaccination. The concept of “playing your cards” engages students as active participants in their health care and promotes healthy coping during vaccinations. Some examples of specific coping interventions that students can select are shown in Figure 1.
Table 1. CARD™ framework for vaccination delivery.
Reprinted with permission from Oxford University Press.
Taddio A, MacDonald N. Addressing vaccine hesitancy in travellers: The CARD™ System. J Travel Med 2019 Sep 2;26(6). pii: taz056. doi: 10.1093/jtm/taz056
Figure 1. Sample interventions from the CARD™ System
The CARD™ System was designed with input from all the relevant stakeholders involved in school-based vaccinations, including students, public health staff, school staff, and parents. A stepwise approach was used to identify needs and preferences, develop tools and resources, and evaluate the impact of implementation (6). In a controlled cluster trial, students in schools implementing CARD™ (vs. control) reported less fear (OR=0.47; 95% confidence interval [CI] 0.27 to 0.82) and dizziness (OR 0.26; 95% CI 0.07 to 0.91). Students in the CARD™ schools had statistically significantly higher knowledge scores and more positive attitudes about vaccination. Additional benefits included the strengthening of relationships between health providers and both students and school staff, and an improved vaccination experience for all stakeholders involved. Readers of this article can refer to the supplement issue of the journal Paediatrics & Child Health dedicated to CARD™ for additional details (6).
CARD™ offers a systematic approach to planning and delivering school-based vaccinations that incorporates student needs and preferences, promoting person-centred care and health equity for all children. The CARD™ framework is transferable across health units and settings providing vaccinations at school, with tailoring to the local context. In summary, addressing student needs and preferences improves the vaccination experience. It also has the potential to promote vaccination and improve health outcomes for children. Of note, CARD™ is also relevant more broadly to managing acute fear and anxiety; we have created an adaptation of CARD™ for the COVID-19 pandemic. The original versions (for school staff, parents, and kids/adolescents) and adapted versions of CARD™ are available on the Immunize Canada website.
References:
- Cooper Robbins SC, Ward K, Skinner SR. School-based vaccination: a systematic review of process evaluations. Vaccine. 2011;29(52):9588-99. doi: 10.1016/j.vaccine.2011.10.033.
- Bucci LM, MacDonald NE, Sondagar C, Taddio A. Taking the sting out of school-based immunizations. Paediatr Child Health. 2017;22(1):41-42. doi: 10.1093/pch/pxx004.
- McMurtry CM, Pillai Riddell R, Taddio A, Racine N, Asmundson GJ, Noel M, Chambers CT, Shah V, HELPinKids&Adults Team. Far from “just a poke”: Common painful needle procedures and the development of needle fear. Clin J Pain 2015;31 (10 Suppl):S3–11. doi: 10.1097/AJP.0000000000000272.
- Taddio A, McMurtry CM, Shah V, Riddell RP, Chambers CT, Noel M, MacDonald NE, Rogers J, Bucci LM, Mousmanis P, Lang E, Halperin SA, Bowles S, Halpert C, Ipp M, Asmundson GJG, Rieder MJ, Robson K, Uleryk E, Antony MM, Dubey V, Hanrahan A, Lockett D, Scott J, Bleeker EV, HELPinKids&Adults. Reducing pain during vaccine injections: clinical practice guideline. CMAJ. 2015 Sep 22;187(13):975-982. doi: 10.1503/cmaj.150391
- WHO. Reducing pain at the time of vaccination: WHO position paper – September 2015. WER 2015;90(39):505-516. http://www.who.int/wer/2015/wer9039.pdf?ua=1
- Taddio A. Pain pain go away: improving the vaccination experience at school. Paediatr Child Health. 2019 Apr;24(Suppl 1):S1-S67. https://academic.oup.com/pch/issue/24/Supplement_1